Arthritis affects around one in five adults in the United States. According to the US Centers for Disease Control (CDC), it is the leading cause of disability and work limitations. The CDC survey also indicates that race and obesity are contributing factors. Non-Hispanic whites are almost 7 to 9 times more likely than African-Americans and Hispanics to have arthritis. The number jumps to 27 times more likely than people with Asian descent.
How is Arthritis Affected by Race?
When looking at race for dietary or medical issues we may consider culture as a key factor. Our diet may be more of a factor than who we descended from. Arguably, race, culture and diet are tightly bound for most people. This notion is enforced by things such as a grandmother’s family recipe or foods traditionally associated with any race or culture. For example, the Hawai’i Journal of Medicine and Public Health found Native Hawai’ians and Pacific Islanders (NHPI) had a higher rate of arthritis than whites. This would indicate a given race was more likely to have arthritis. However, the authors state “Obesity may be a contributing factor, since obesity rates were significant higher in NHPI males and females.” In the study and the CDC’s work, the only consistent factor is obesity.
Looking into the Hawai’ian diet, we may think of a tropical paradise with a plethora of native and imported flora and fauna to augment our daily food choices. However, the rapidly increasing population has resorted to importing most food products (85-90%) from the industrialized mainland US and others. In reality, the modern Hawai’ian diet is heavily infused with the industrial diet that many blame for degrading health on an institutional level. Just google “spam recipes in Hawaii” if you don’t believe us!
Is Arthritis Affected by Diet?
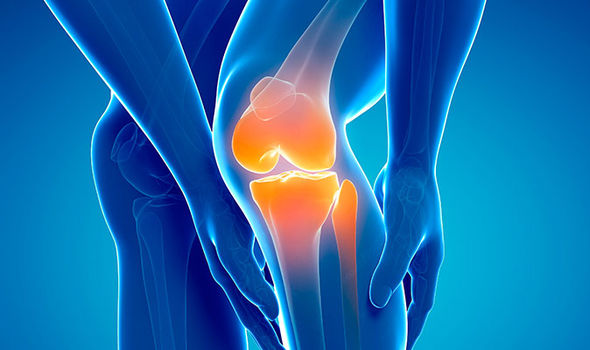
At Tarsul we are constantly on the lookout for diet as a touch-point for fighting diseases. With arthritis, joint pain is caused by more weight on our joints among other factors. This seems to reinforce the body mass index to diagnosed with arthritis correlation. Additionally, this Harvard Medical School article and others firmly link diet to osteoarthritis and rheumatoid arthritis. Unfortunately, only glucosamine and chondroitin sulfate may decrease pain in people with moderate to severe osteoarthritis of the knee. They do not help people with rheumatoid arthritis. For arthritis treatments, this leaves the field wide open with no winners in sight.
Interestingly, both of Tarsul’s ingredients can be used to target inflammation and joint pain. Scientific literature suggests that MSM (organic sulfur) may have clinical applications for arthritis and other inflammatory disorders such as interstitial cystitis, allergic rhinitis, and acute exercise-induced inflammation. Ingesting cream of tartar (potassium bitartrate) leverages the information that an increase in potassium can decrease pain intensity. Additionally, Tarsul can address the body’s needs for sulfur and potassium which affects a number of other symptoms and diseases. Overall, dietary changes supplemented by Tarsul can produce health benefits including a decrease in pain and inflammation; the main symptoms of arthritis.